PLANTAR FASCIITIS
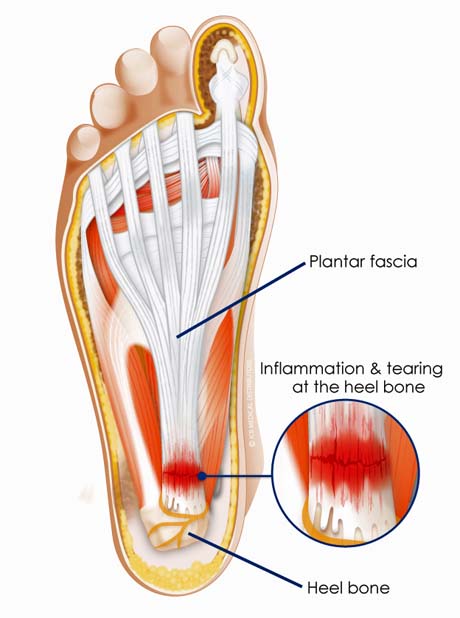
Plantar fasciitis. The red circle indicates the point of pain
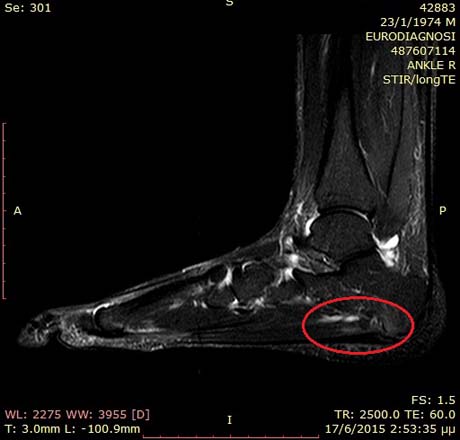
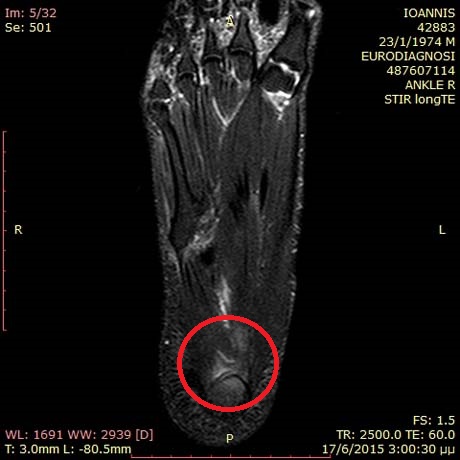
Foot MRI: inflamation point due to plantar fascitis (red cyrcle)
Plantar heel pain may be caused by a variety of conditions, the most common of which is proximal plantar fasciitis or heel pain syndrome. The plantar fascia is a dense sheet of connective tissue that originates from a medial calcaneal tuberosity and inserts in multiple slips on the bases of the proximal phalanges and flexor tendon sheaths.
CAUSE
The etiology of plantar fasciitis is not well understood but is generally thought to be related to degeneration and microtearing of the origin of the plantar fascia at the medial calcaneal tuberosity.
An acute injury may be the precipitating event that initiates the process of inflammation and injury at this location, but frequently no specific traumatic event can be recalled. Calcaneal spurs, however may form as a result of chronic periostitis of the calcaneus at the origin of the plantar fascia.
Approximately 10% of patients will develop persistent disabling symptoms.
SYMPTOMS
- Patients typically report pain that is worse for the first few steps upon arising in the morning. This is thought to be a result of the equinus posturing of the foot during sleep and the resulting microtearing and inflammation than is reinitiated with the first few steps in the morning.
- Pain is also worse upon rising after long periods of rest.
- Obesity, occupations involving prolonged standing, long distance running, or hyperpronated feet have all been associated with plantar fasciitis.
EXAMINATIONS
- On physical examination, there is maximal tenderness at the medial plantar aspect of the calcaneal tuberosity. This is the most important finding in making a diagnosis of proximal plantar fasciitis.
- Radiographs may reveal the presence of a calcaneal spur. The absence of the spur not exclude the diagnosis of disease.
Calcaneal spur
- Magnetic resonance imaging of the foot reveals the anatomical details of soft tissue.
'Heel spur, which is the result of chronic plantar fasciitis which causes intense pain to the patient
PRP - GROWTH FACTORS PLATELET RICH PLASMA
PRP - PLATELET REACH PLASMA




